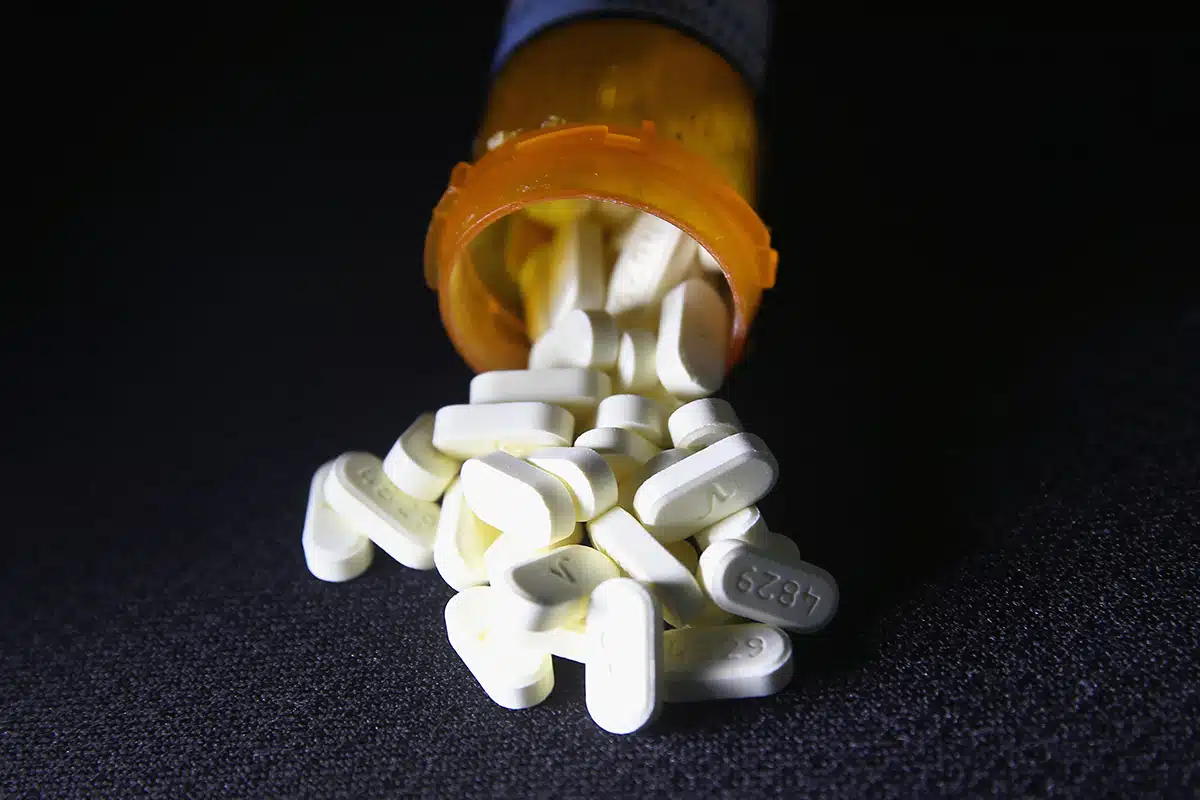
Consider Alternatives to Pain Relief — Although opioids are the most ubiquitous response to treating pain today, they have limited long-term efficacy data and are known to cause abuse, addiction, and death.
In 1999, the Joint Commission, which accredits more than 21,000 US healthcare organizations and programs, made pain the “fifth vital sign,” recognizing the problem of uncontrolled pain. However, they did not give physicians the tools to provide pain control safely and effectively. Rather, the medical community indicated to patients and physicians alike that patients would not become addicted to opioids, that opioids were safe and universally effective.
Today, patients are still hurting. It is not enough to simply tell physicians to avoid opioids, as has been suggested by the “CDC Guideline for Prescribing Opioids for Chronic Pain.” Pain treatment requires a nuanced approach. It is important to put the risks of opioids into an appropriate context, and to offer alternative treatment strategies to those suffering with acute and chronic pain.
Innovation will become ever more critical as we combat the opioid crisis. Many times, there are interventional therapies that physicians could and should employ before prescribing opioids. Conventional techniques, such as facet blocks, radiofrequency ablation, and other routine injections, have been around for decades and often are effective at reducing pain and opioid use while improving function. It is important that insurers recognize these approaches and not dismiss them as experimental.
These therapies should be used as a first line of defense, earlier in the pain treatment continuum, long before opioid use transforms into abuse. When earlier interventions — such as physical therapy, over-the-counter medications, or a short course of low-dose opioid therapy — fail, those patients should be referred to interventional pain specialists who have greater training and can consider a vast array of therapies as replacements for, or to minimize the use of, opioids.
The BIMC Pain Management Centre offers radio frequency ablation, epidural steroid injections, nerve blocks and joint injections. Your pain management timeline will vary depending on your condition, but most BIMC patients can expect to go through these steps:
Diagnose the cause of your pain
The most important step in pain management is to find the right diagnosis. A pain management doctor can determine the diagnosis from a patient’s signs and symptoms, physical examination, additional examinations (x-ray, CT-scan, MRI, etc.), even perform diagnostic minimal invasive procedures such as test injections.
Discuss potential therapies that could help
After diagnosing your pain, a pain management doctor will review available therapies for your condition and discuss the one that works best for you. All the risks and benefits of any procedure or therapy can be considered at this stage.
Coordinate care between multiple healthcare professionals
The process of pain management can involve more than one doctor. The pain management doctor will coordinate care with other specialty doctors to serve the patient’s best interest.
Performs any necessary interventional procedure
A pain management doctor also has special training to perform minimal invasive procedures, which could be perhaps an injection at the source of pain, usually with ultrasound or fluoroscopy guidance.