Interventional Pain Management — A report released in April by Research & Markets points out that the global opioids market size is growing at a staggering pace in Asia Pacific largely due to increasing geriatric population, coupled with a focus on palliative care. And rising prevalence of disease conditions with chronic pain, such as cancer, lower back pain, arthritis, and fibromyalgia, is also driving the opioids market.
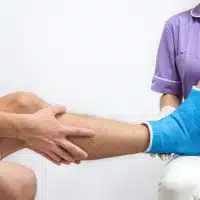
The BIMC Siloam Nusa Dua Pain Clinic has treated a growing number of people with chronic pain, which affects all aspects of their lives. Patient surveys show those with chronic pain care about more than just experiencing less pain; what matters is enjoying life, having a strong sense of emotional well-being, improving sleep as well as participating in social and recreational activities. These goals need to be balanced against the downsides of pain treatment like opioid use.
For example, opioid medications may reduce pain intensity and make it easier to fall asleep however they also make people tired, cause constipation and memory problems, and carry the risk of abuse and overdose. How the benefits and harms are balanced vary from patient to patient.
For some people, the risk of abuse is small, the side effects are minor, and the drug reduces their pain significantly. For others, these drugs reduce pain only a little, while the fatigue and cognitive side effects are so bad that it is hard to carry out routine activities like driving or going to work.
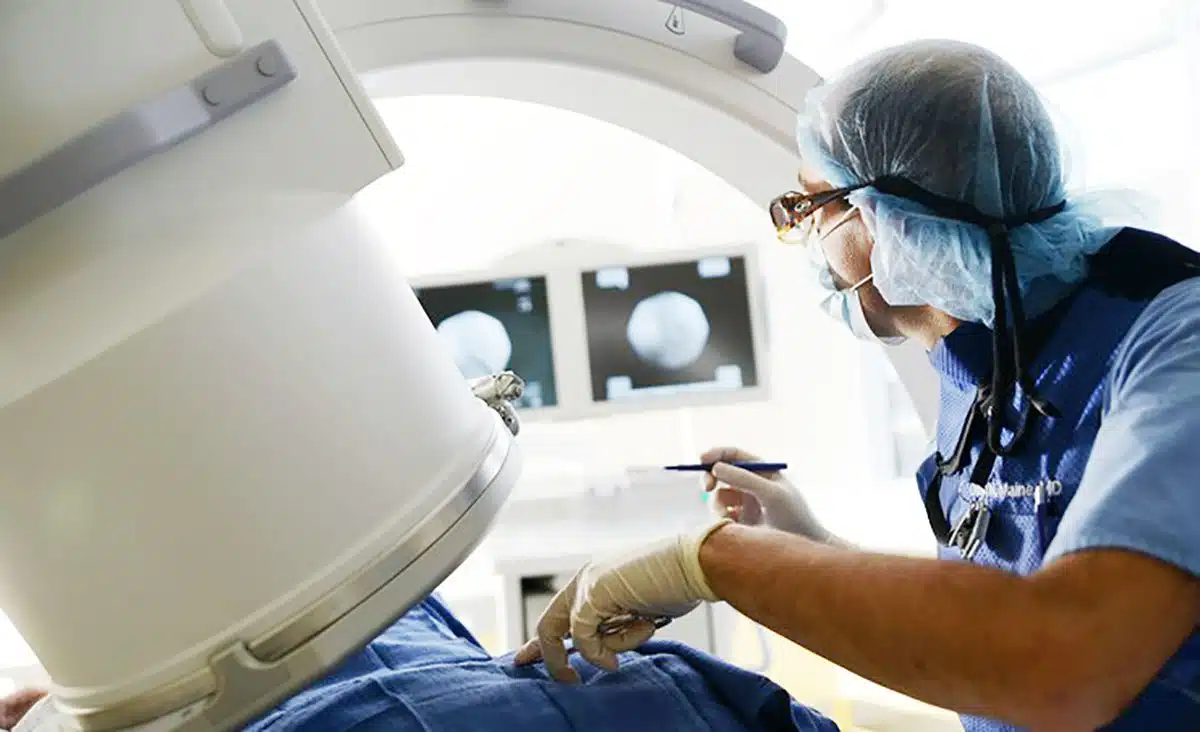
The future of pain-management treatments, also called “interventional” pain management, has shown success for chronic pain and takes a multimodal approach by using a combination of injections, stimulation, pain pumps, and other treatments.
BIMC Siloam Nusa Dua’s pain interventionist, Dr. Cindy, says what makes interventional pain management different is that it uses techniques, such as injections and radiofrequency rhizotomy, to directly address the source of your pain. She says some conditions commonly treated include: chronic headaches, mouth, or face pain; low back pain; muscle and/or bone pain and neck pain. By using a combination of therapies, patients receive the most benefits with the fewest harms.
Overall, pain intervention helps meet quality-of-life goals — along with a renewed focus on individualized treatment — critical steps towards more effectively fulfilling our duties to suffering patients. We determine a patient’s symptoms and complaints by physical examination and investigations that could start by way of x-rays or CT scans, minimally invasive diagnostic actions followed by providing personal treatment options.
Advantages and disadvantages of the therapy are explained by our specialists and may include “multi-profession care coordination,” a process of therapy involving more than one specialist or “intervention action” drawing in epidural steroid injections, nerve blocks and radiofrequency ablation.