About 50 per cent of Indonesia’s population is at risk of malaria, with the most affected area in the eastern parts of Indonesia, from East Nusa Tenggara to Maluku and Papua.
The areas covering Sumatera, Kalimantan and Sulawesi are considered to have medium levels of malarial transmission whereas Bali and Jakarta have zero to low levels of malaria. However, travelers who have recently visited the Gili Islands (Lombok, West Nusa Tenggara) are at risk of possible malarial infection.
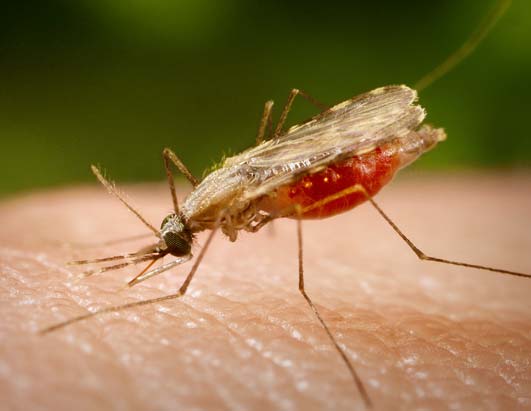
Human malaria is caused by four different species of the protozoan parasite Plasmodium: P. falciparum, P. vivax, P. ovale, and P. malaria. The malaria parasite is transmitted by various species of the Anopheles mosquito, which bite mainly between sunset and sunrise (night time) and is more likely to be found in forested and swampy areas. The incubation period is 7 days or longer.
Following the bite of an infected female Anopheles mosquito, the inoculated sporozoites infect the liver within 1 to 2 hours. Individuals are asymptomatic for 12 to 35 days (depending on parasite species), until the erythrocytic stage of the parasite life cycle. Release of merozoites from infected red cells when they rupture causes fever and other manifestations of malaria.
The relapsing species Plasmodium vivax and P. ovale can present as a new infection weeks or months after the initial illness due to activation of residual hypnozoites in the liver.
The initial symptoms of malaria are nonspecific and may overlap with other clinical presentations (such as upper respiratory tract infection or gastrointestinal illness). The symptoms include fever, chills, malaise, fatigue, diaphoresis, headache, cough, anorexia, nausea, vomiting, abdominal pain, diarrhea, arthralgia, and myalgia.
A blood sample should be examined to test for the malaria parasite. If no parasites are found in the first blood film while there is clinical suspicion of malaria, a series of blood samples should be taken at 12-24 hours intervals and examined very carefully.
Prompt and accurate diagnosis of malaria is needed for implementation of appropriate treatment to reduce associated morbidity and mortality.
In Indonesia, malaria is resistant to traditional treatment such as chloroquine and sulphadoxine-pyrimethamine. Since 2004, ACT (Artemisin Combination Therapy) has been a standard treatment for malaria in Indonesia. The relatively higher cost of Artemisin Combination Therapies (ACTs) makes a laboratory diagnosis of malaria more cost effective than empiric therapy.
No antimalarial prophylactic regimen gives complete protection but good chemoprophylaxis (adherence to the recommended drug regimen) does reduce the risk of fatal disease.
The following should also be taken into account about antimalarial prophylaxis:
- Dosing schedules for children should be based on body weight.
- Antimalarials that are taken daily should be started the day before arrival in the area of prevalence.
- Weekly mefloquine should be started at least 1 week, although preferably 2-3 weeks, before departure, to achieve higher pre travel blood levels and to allow side effects to be detected before travel.
- Antimalarial drugs must be taken with food and swallowed with plenty of water.
- Antimalarial drugs should be continued for 4 weeks after the last possible exposure to infection, since parasites may still emerge from the liver during this period. The single exception is atovaquone /proguanil, which can be stopped 1 week after returning from travels.
Preventing mosquito bites:
- Avoid outdoor exposure between dusk and dawn (when Anopheles mosquitoes feed).
- Wear clothing that reduce the amount of exposed skin.
- Use insect repellant.
- Use mosquito nets above your bed.
- Stay in well-screened or air-conditioned spaces.